Psychedelic_integration_An_anal… “Psychedelic Integration: An Analysis of the Concept and Its Practice” (Bathje et al., 2022)
Psychedelic Integration: What It Really Means (And Why It Matters)
In recent years, psychedelics have returned to mainstream conversation — in therapy rooms, research labs, wellness spaces, and spiritual communities. But alongside the renewed interest in substances like psilocybin, MDMA, and ayahuasca, one word keeps appearing:
Integration.
Everyone says it’s important. But what does it actually mean?
A 2022 paper by Geoff Bathje and colleagues offers the first comprehensive attempt to clarify the concept. Their work reviews dozens of definitions, models, and practices and proposes a unified way of understanding what psychedelic integration really involves.
Here’s what they found.
What Is Psychedelic Integration?
Across many sources, integration is described as:
Making sense of a psychedelic experience
Working through difficult or confusing material
Translating insights into real-life changes
Incorporating lessons into daily living
The authors synthesize these ideas into a clear definition:
Integration is an active process of revisiting, processing, and incorporating the lessons of a psychedelic experience into one’s life in ways that promote balance and wholeness.
In other words:
The journey doesn’t end when the substance wears off. In many ways, that’s when the real work begins.
Why Integration Is Necessary
There’s a common misconception that psychedelics “do the healing” for you. The research reviewed in this paper suggests otherwise.
Psychedelics may:
Open insight
Increase psychological flexibility
Reveal unconscious material
Create powerful emotional or spiritual experiences
But without intentional follow-up:
Insights fade
Old patterns reassert themselves
Challenging experiences remain unresolved
Integration is what turns insight into lasting change.
Indigenous vs. Western Approaches
One of the most interesting parts of the article explores cultural differences.
Indigenous traditions
In many Indigenous cultures, psychedelic use occurs within ritual, community, and holistic worldviews. Healing is not compartmentalized. Mind, body, spirit, community, and nature are interconnected.
In these contexts, “integration” may not even be a separate phase — it’s built into daily life.
Western contexts
Western societies, influenced by dualistic thinking (mind vs. body, individual vs. nature), tend to separate experiences from daily life. As a result, Western participants often need explicit integration practices to bridge the gap.
This cultural difference helps explain why integration has become such a focus in modern psychedelic therapy.
Two Main Models of Integration
The paper identifies ten formal models of integration, which fall roughly into two categories:
1. Psychotherapy-Based Models
These draw from frameworks like:
Acceptance and Commitment Therapy (ACT)
Jungian psychology
Transpersonal psychology
Harm reduction approaches
They focus primarily on:
Meaning-making
Emotional processing
Behavior change
Psychological flexibility
These models are especially useful for clinical populations.
2. Holistic / Biopsychosocial-Spiritual Models
These go beyond the mind and address multiple domains of life:
Mental and emotional
Bodily and somatic
Spiritual and existential
Relational and communal
Lifestyle and action
Nature and environment
These models suggest that psychedelic experiences often reveal imbalance across all these areas — not just psychological distress.
Integration, therefore, means restoring balance across your whole life.
The Authors’ Synthesized Model
After reviewing the literature, the authors propose a unified framework with six domains:
Mind and emotions
Body and somatic experience
Spiritual/existential meaning
Relationships and community
Lifestyle and action
Connection with nature
Effective integration, they argue, should address all six — not just one.
Over-focusing on cognition or therapy alone may reinforce the very imbalances psychedelics sometimes reveal.
What Does Integration Actually Look Like?
The paper compiles a large list of practices used in integration work. These include:
Reflective practices
Journaling
Meditation
Therapy
Meaning-making exercises
Creative expression
Art and drawing
Music
Dance
Writing
Somatic practices
Yoga
Breathwork
Exercise
Massage
Spiritual practices
Ritual
Prayer
Intention-setting
Dreamwork
Nature-based practices
Time outdoors
Hiking
Mindful walks
Community and relationships
Sharing circles
Boundary setting
Service and activism
The point isn’t to do everything. It’s to create a balanced approach that fits your experience and life context.
Key Takeaways
Here are the most important insights from the paper:
Integration requires active effort. Insights do not automatically translate into change.
It is often long-term. Some meanings unfold over months or years.
Balance matters. Mental health frameworks are helpful but incomplete.
Community is protective. Supportive relationships strengthen integration.
Change should be gradual. Big insights often require incremental action.
A Larger Question
The authors close with a broader reflection: Western culture may attempt to assimilate psychedelics into existing structures — capitalism, medicine, productivity — rather than allowing them to reshape those structures.
Integration, then, is not only personal. It may also be cultural.
How do we allow profound experiences to transform our lives — instead of squeezing them back into the old containers?
Final Thought
Psychedelic integration is not a checklist. It is not a brief aftercare session. And it is not just therapy homework.
It is an ongoing process of becoming more whole — mentally, physically, spiritually, relationally, and ecologically.
The psychedelic experience may open the door.
Integration is how you walk through it.
Blog Post: Date
“Prevalence and associations of challenging, difficult or distressing experiences using classic psychedelics” (Simonsson et al., 2023)
Challenging Psychedelic Experiences: How Common Are “Bad Trips,” Really?
Psychedelics are often discussed in terms of healing, insight, and transformation — and growing clinical research suggests they may help treat conditions like depression when used carefully.
But another important question remains:
How often do people have difficult or distressing psychedelic experiences — and what increases the risk?
A 2023 study published in the Journal of Affective Disorders examined exactly that, using a nationally representative sample of U.S. adults. The findings provide one of the clearest pictures so far of how common challenging psychedelic experiences are — and what factors make them more likely.
Here’s what the research shows.
Why Study Difficult Psychedelic Experiences?
While clinical trials typically emphasize safety and positive outcomes, they occur in carefully controlled environments with:
Screening procedures
Psychological preparation
Supportive settings
Trained facilitators
Outside those conditions, experiences can vary widely.
Researchers wanted to understand:
How often people encounter distressing psychedelic experiences
Whether certain medications increase risk
How “set and setting” influence outcomes
The real-world prevalence of negative effects
How the Study Worked
Researchers surveyed:
2,822 U.S. adults (representative by age, sex, and ethnicity)
Among them, 613 people who reported lifetime use of classic psychedelics such as LSD, psilocybin, DMT, or mescaline.
Participants answered detailed questions about:
Difficult or distressing psychedelic experiences
Functional impairment
Long-term symptoms
Environmental and psychological factors during the experience
Medication use
Whether harm or medical intervention occurred afterward
How Common Are Challenging Experiences?
The findings challenge some common assumptions.
Most people did NOT report distressing experiences.
59.1% said they had never had a challenging or distressing psychedelic experience.
However:
About 41% reported at least occasional difficulties.
8.9% experienced impairment lasting longer than one day.
Around 4.6% reported severe functional impairment.
So while serious issues are not the norm, they are also not rare.
What About Long-Term Effects?
Many participants reported lingering symptoms lasting at least several days, including:
Anxiety
Sleep difficulties
Trouble thinking clearly
Feeling disconnected from others or reality
Importantly, despite difficult experiences:
👉 Most respondents still agreed they were glad they had used psychedelics overall.
This reflects a recurring theme in psychedelic research: challenging experiences may still be interpreted as meaningful or beneficial afterward.
Risk of Harm: How Often Does It Happen?
More serious outcomes were relatively uncommon but notable:
6.7% reported thoughts or attempts of harming themselves or others after a difficult experience.
2.6% sought medical, psychiatric, or psychological assistance afterward.
These numbers highlight that while risks are relatively low at the population level, they are significant enough to warrant attention.
The Biggest Risk Factors: Set and Setting
One of the strongest findings involved “set and setting” — the psychological state and environment surrounding the experience.
Factors linked to more difficult experiences included:
No preparation beforehand
Negative mindset going in
Lack of psychological support
Disagreeable physical environment
Taking too high a dose
Experiencing a major life stressor beforehand
These findings reinforce decades of psychedelic research emphasizing that context strongly shapes outcomes.
Medication Interactions Matter
Another key result involved medication co-use.
Higher risk was associated with:
Lithium
Other mood stabilizers
These combinations were linked to:
More intense challenging experiences
Increased risk of harm
This supports existing safety guidelines recommending caution or exclusion of certain medications in clinical settings.
What Helps During a Difficult Experience?
Participants reported several strategies that helped manage challenging moments:
Trying to calm the mind
Changing physical location
Asking friends for support
Altering the social environment
Interestingly, calming practices like mindfulness or grounding techniques appear particularly helpful — suggesting preparation may include learning emotional regulation tools.
What This Means for Harm Reduction
The study reinforces several practical lessons:
Psychedelics are not inherently safe or unsafe — outcomes depend heavily on context.
Preparation and support significantly reduce risk.
Screening for medication interactions is important.
Difficult experiences are common but usually manageable.
A small minority may require professional assistance afterward.
Limitations to Keep in Mind
The authors note important limitations:
The study cannot prove cause-and-effect relationships.
Data relied on self-reporting.
Participants may not represent all demographic factors.
Future research will need longitudinal designs to better understand long-term outcomes.
Final Thought
As psychedelic use grows — whether in clinical therapy, personal exploration, or spiritual practice — understanding risks is just as important as celebrating benefits.
This study adds nuance to the conversation:
Most people do not experience severe distress, but context matters profoundly.
Mindset, environment, preparation, and support are not secondary details — they may be the difference between a transformative experience and a difficult one.
Blog Post: Date
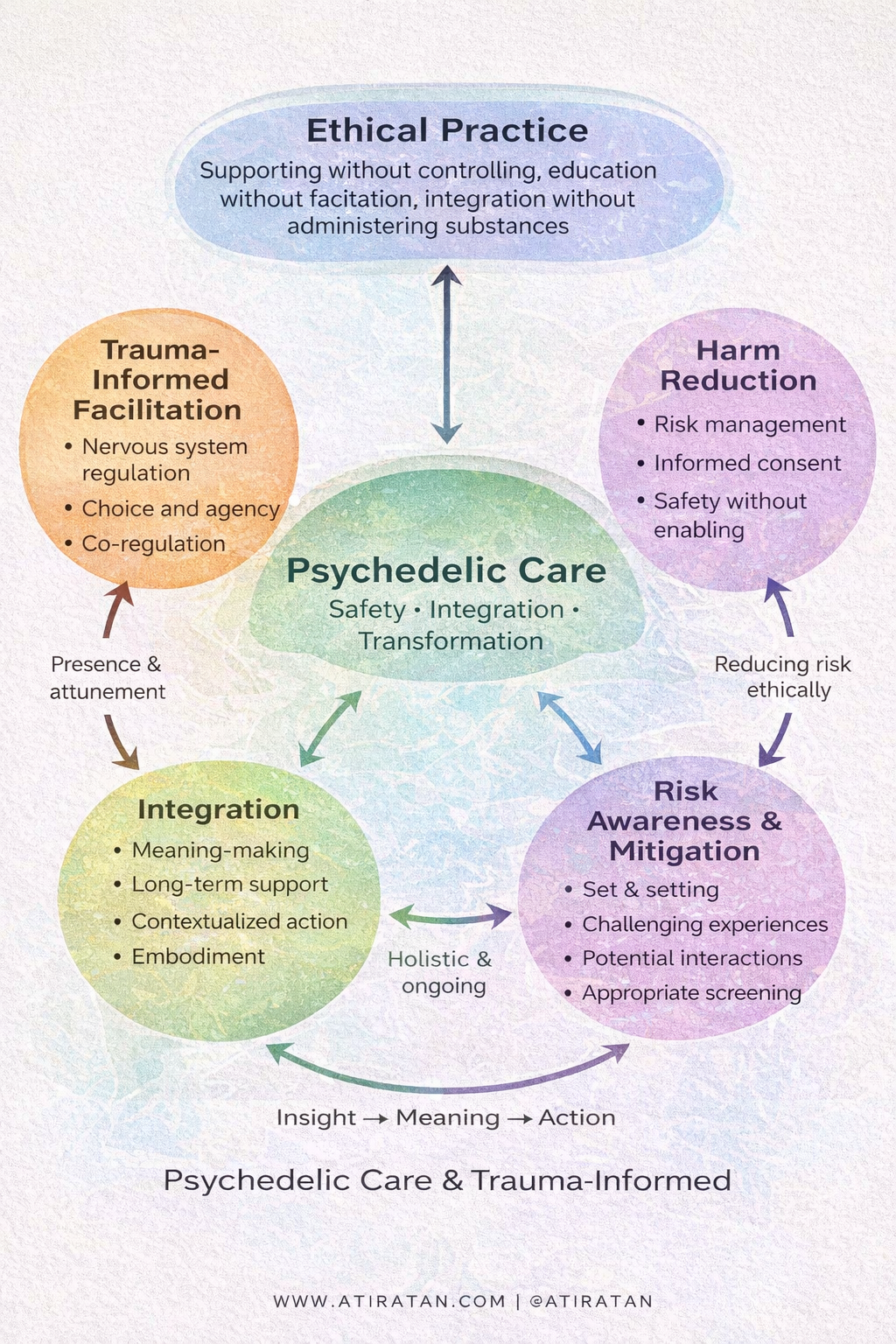
Psychedelic Care & Trauma-Informed Practice
Part 1 — Psychedelic Experiences Don’t End When the Journey Ends
Modern psychedelic research increasingly shows that the experience itself is only one part of the process.
Integration — the ongoing work of making meaning and translating insights into life — is where lasting change happens. Integration involves multiple domains:
psychological reflection
emotional processing
body awareness
relationships
lifestyle change
spiritual meaning-making
Without preparation and integration, powerful insights may fade or even become destabilizing.
Part 2 — The Reality of Challenging Psychedelic Experiences
Popular culture sometimes frames psychedelics as inherently healing — but research paints a more nuanced picture.
Large population studies show:
Most people do not experience severe distress.
However, challenging experiences are common.
A small but meaningful percentage experience functional impairment or require support afterward.
What predicts difficulty?
👉 Not just the substance — but set and setting:
negative mindset
lack of preparation
insufficient psychological support
stressful life events
excessive dosage
This reinforces a key principle:
Psychedelic safety is relational and contextual, not purely pharmacological.
Part 3 — Ethical Practice in a Complex Legal Landscape
As interest in psychedelics grows, therapists and facilitators face a unique challenge:
Clients may pursue psychedelic experiences independently — often outside legal frameworks.
Harm reduction and integration therapy provide an ethical middle path:
support without promoting illegal activity
education without facilitation
integration without administering substances
This approach prioritizes:
autonomy
safety
informed decision-making
ethical boundaries
The role of the facilitator shifts from guide of the experience to guide of reflection and integration.
Part 4 — Trauma-Informed Facilitation: The Foundation Beneath It All
Across all psychedelic work, trauma-informed practice emerges as essential.
Trauma-informed facilitation emphasizes:
nervous system awareness
restoration of choice and agency
relational safety and co-regulation
Rather than focusing only on techniques, the facilitator learns to:
track regulation states (social engagement, hyper-arousal, hypo-arousal)
offer options instead of directives
use presence, tone, and pacing to support safety
Transformation becomes possible not because of intensity — but because participants feel resourced enough to stay present.
Blog Post: Date
The Four Core Pillars of Psychedelic Care
1. Transformation Requires Integration
Insight alone does not create change.
Integration bridges:
experience → meaning → action → embodiment
This process is holistic and ongoing.
2. Risk Is Real — But Context Shapes Outcomes
Psychedelics are neither inherently safe nor dangerous.
Risk increases when:
preparation is lacking
emotional support is absent
individuals are destabilized beforehand
medication interactions are ignored
Safety emerges from relational care and environment.
3. Ethical Practice Means Supporting Without Controlling
The modern facilitator operates within ethical tension:
respecting autonomy
maintaining legal boundaries
reducing harm without enabling unsafe behavior
This requires clarity of role and strong professional boundaries.
4. The Nervous System Is the Real “Setting”
Trauma-informed perspectives reveal that the deepest layer of set and setting is internal regulation.
Key insights:
Trauma often reflects loss of agency → facilitators restore choice.
Co-regulation is faster than self-regulation.
Presence and attunement matter as much as technique.
Ultimately, the facilitator’s regulated nervous system becomes one of the most powerful tools in the room.
Big Picture
Psychedelic work is not just about altered states — it is about regulated relationships, ethical frameworks, and embodied integration.
The most effective approach combines:
trauma-informed care
harm reduction principles
ethical awareness
long-term integration support
When these elements come together, psychedelic experiences can move beyond moments of intensity and become sustainable pathways for growth.
Blog Post: Date